The effects of Shilajit on periodontal ligament cells in wound healing: a comprehensive in vitro study – PubMed Black Hawk Supplements
BLACK HAWK: Most trusted lions mane supplement for adrenal fatigue
Published article
CONCLUSIONS: Our research offers novel proof that shilajit promotes hPDL cell migration and proliferation, which in turn promotes wound closure. According to these results, Shilajit may improve tissue regeneration, accelerate wound healing, and encourage the growth of periodontal ligament cells.
Black Hawk Supplements, best supplements in the UK

The effects of Shilajit on periodontal ligament cells in wound healing: a comprehensive in vitro study
Abdullah Alqarni et al. BMC Complement Med Ther. .
Abstract
Background: Shilajit is a pale-brown to blackish-brown fluid that varies in consistency and is released from rock layers in various mountain ranges across the world. For thousands of years, traditional medical systems in several nations have included shilajit in one form or another as a rejuvenator and adaptogen. Numerous medicinal qualities have been attributed to it, several of which have been confirmed by contemporary scientific analysis. This in vitro study was established to investigate the effect of shilajit on human Periodontal ligament (hPDL) cell wound closure.
Methods: The cell viability was evaluated using the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide tetrazolium reduction (MTT) test following a 24-hour exposure of shilajit. With the use of an inverted phase contrast microscope, morphological alterations were noted. Acridine orange/ethidium bromide dual labeling, to evaluate the apoptotic cell death in shilajit treated cells. An in vitro wound healing test was utilized to evaluate wound healing in wounded hPDL cell monolayers for 24 h in the presence or absence of shilajit. The Matrix metalloproteinases-2 and 9 (MMP-2 and MMP-9) in hPDL cells treated with shilajit were measured using the enzyme-linked immunosorbent assay (ELISA) technique, and real-time PCR was used to examine gene expression linked to wound healing and apoptosis.
Results: Shilajit’s cytotoxicity evaluation on hPDL cells showed that dosages as high as 3 mg/mL had no adverse effects and maintains the cell viability, suggesting a possible stimulatory effect on cell growth. Cell viability was reduced significantly (p < 0.05) by dosages more than 4 mg/mL, indicating cytotoxicity at higher concentrations. According to the scratch wound healing assay, shilajit administration at doses of 2 and 3 mg/mL accelerated wound healing and improved cell migration in hPDL cells. Shilajit promoted a controlled inflammatory response and supported periodontal ligament healing by upregulating the expression of genes involved in collagen synthesis, collagen type I alpha 1 chain (COL1A1) and pro-inflammatory cytokines, tumor necrosis factor alpha (TNF-α) and, interleukin-1-beta (IL-1β), according to real-time PCR data. In addition, Shilajit raised the protein levels of MMP2 and MMP9, two important enzymes involved in tissue remodeling. Shilajit-treated hPDL cells showed a substantial increase of cell proliferation and no discernible apoptotic activity.
Conclusions: Our research offers novel proof that shilajit promotes hPDL cell migration and proliferation, which in turn promotes wound closure. According to these results, Shilajit may improve tissue regeneration, accelerate wound healing, and encourage the growth of periodontal ligament cells.
Keywords: Migration; Periodontal ligament cells; Proinflammatory cytokines; Shilajit; Wound closure.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study was conducted according to the guidelines of the Declaration of Helsinki. The Research Ethics Committee, College of Dentistry, King Khalid University has reviewed and approved the research with a reference no: IRB/KKUCOD/ETH/2023-24/011. All methods were performed in accordance with the relevant guidelines/regulations/legislation. Commercially available 200 mg Himalayan Shilajit paste (Lajit, USA) was purchased and used in the current study. Informed consent to participate in the study was obtained from the participants. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
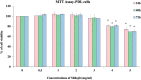
The cytotoxic effects of Shilajit (0.5 to 5 mg/ml) on hPDL cells. Cells were treated for 24 h, 48 h and 72 h, and cell viability was evaluated by MTT assay. Data are shown as means ± SD (n = 3). * compared with the control blank group, p < 0.05

Effect of Shilajit on cell morphology of human hPDL cells. Cells were treated with Shilajit (2, 3 and 4 mg/ml) for 24 h along with the control group. Images were obtained using an inverted phase contrast microscope

In vitro scratch wound healing assay. Human hPDL cells were injured and cell migration assay with and without treatment of Shilajit (2 and 3 mg/ml) was performed for 24 h. Images were obtained using an inverted Phase contrast microscope
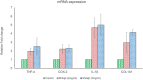
Effect of Shilajit (2 and 3 mg /ml) on TNF-a, COX-2, IL-1B and COL1A1 gene expression in hPDL cells. Target gene expression is normalized to GAPDH mRNA expression and the results are expressed as fold change from control. Each bar represents the mean ± SEM of three independent observations. ‘*’ represents statistical significance between control versus drug treatment groups at p < 0.05 level

MMP2 and MMP9 levels in hPDL cells were assessed by ELISA kit. The condition media was used from control and Shilajit 2 and 3 mg/ml treated cells. Each bar represents the mean ± SD. *Statistically significant difference between two groups (p < 0.05); #statistically significant difference between control and treated (p < 0.05)
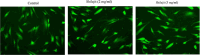
Human hPDL cells were treated with Shilajit (2 and 3 mg/ml) for 24 h along with the control group. After the treatment, the cells were incubated with AO/EtBr dual staining. Images were obtained using an Inverted Fluorescence Phase contrast microscope
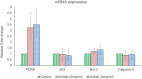
Effect of Shilajit (2 and 3 mg /ml) on Proliferative marker gene (PCNA) and Apoptotic genes (p53, Bcl-2, Caspase-3) expression in hPDL cells. Target gene expression is normalized to GAPDH mRNA expression and the results are expressed as fold change from control. Each bar represents the mean ± SEM of three independent observations. ‘*’ represents statistical significance between control versus drug treatment groups at p < 0.05 level
References
-
- Nuñez J, Vignoletti F, Caffesse RG, Sanz M. Cellular therapy in periodontal regeneration. Periodontol 2000. 2019;79:107–16. – PubMed
MeSH terms
Substances
BLACK HAWK: Best shilajit supplement for elderly
Read the original publication: